It can be a surprising and even frightening moment. One second, your hands look completely normal. The next, you notice that one or more of your fingers have turned an unusual color—chalky white, pale yellow, or even bluish-purple. At first, you might assume it’s just the cold, especially during winter. But what if it keeps happening, even when the temperature doesn’t feel that low?
If your fingers change color when you hold a cold drink, wash your hands, or feel stressed, the cause may be more than just chilly weather. According to medical experts, these episodes could be a sign of a condition called Raynaud’s disease, also known as Raynaud’s phenomenon.
What Is Raynaud’s Disease?
Raynaud’s disease is a condition that affects blood circulation, most often in the fingers and toes. In some cases, it can also affect the ears, nose, lips, or even the nipples. During a Raynaud’s episode—often called an “attack”—the small blood vessels in these areas suddenly tighten and narrow. This limits blood flow and causes noticeable changes in skin color.
These color changes often follow a familiar pattern:
- White: Blood flow is reduced, causing the skin to lose its normal color.
- Blue: With less oxygen reaching the area, the skin may turn bluish.
- Red: As blood flow returns, the skin may flush red and feel warm, tingly, or sore.
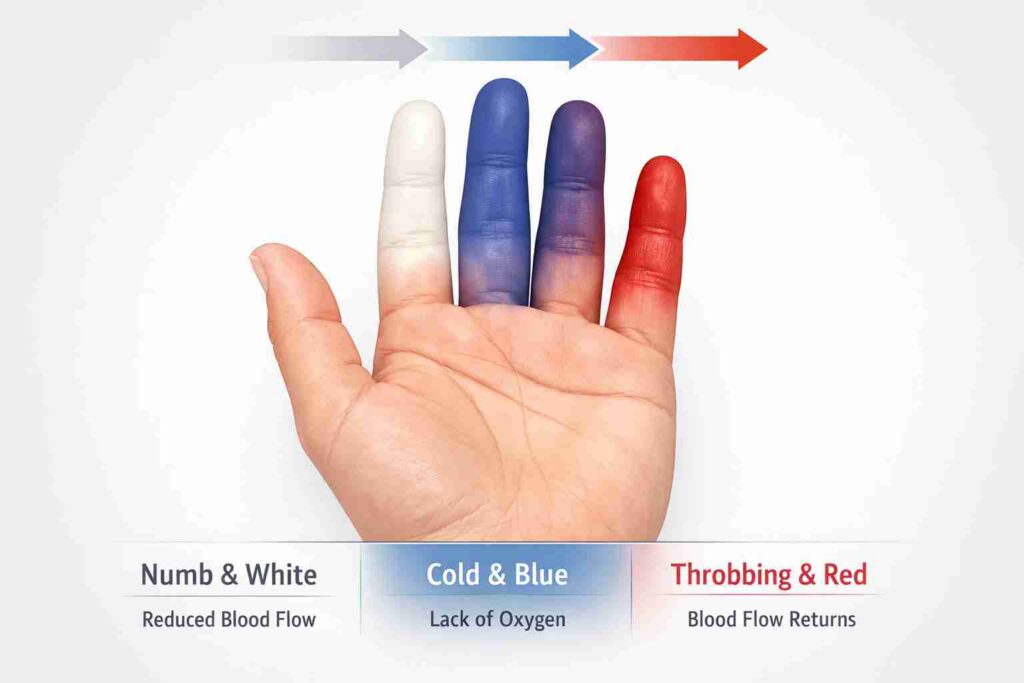
Not everyone experiences all three stages. Some people may only notice one or two color changes, but repeated episodes are still important to pay attention to.
Why Do Raynaud’s Episodes Happen?
The two most common triggers for Raynaud’s are cold temperatures and emotional stress. Even small temperature changes can bring on an episode, such as:
- Holding a cold can or glass
- Reaching into a freezer
- Washing hands in cold water
- Stepping from a warm building into cool outdoor air
Stress and anxiety can also trigger symptoms. When you feel tense, your body may respond by tightening blood vessels, much like it does in cold conditions. Experts believe Raynaud’s involves an exaggerated response from the nervous system that controls blood vessel narrowing.

Primary vs. Secondary Raynaud’s
Doctors generally classify Raynaud’s into two types:
Primary Raynaud’s (Raynaud’s Disease)
This is the most common and usually milder form. It occurs on its own and is not linked to another medical condition. Symptoms often begin in the teen years or early adulthood. While the episodes can be uncomfortable or alarming, primary Raynaud’s rarely causes long-term damage.
Secondary Raynaud’s (Raynaud’s Phenomenon)
This form is linked to another underlying condition, often involving connective tissue or blood vessels. Secondary Raynaud’s tends to be more severe and may lead to complications if left untreated. Because of this, doctors take it more seriously and often recommend further testing.
What Does Raynaud’s Feel Like?
Along with noticeable color changes, Raynaud’s episodes may cause:
- Cold or icy sensations in fingers or toes
- Numbness or tingling
- A pins-and-needles feeling as circulation returns
- Mild to moderate pain in some cases
For many people, the most unsettling part isn’t the discomfort—it’s how suddenly and dramatically the hands or feet change color.
Is Raynaud’s Dangerous?
For most people with primary Raynaud’s, the condition is more inconvenient than dangerous. Episodes are temporary, and normal color and sensation usually return once the trigger is removed.
However, frequent or severe attacks—especially those involving pain, sores, or slow healing—should not be ignored. In rare cases, prolonged loss of blood flow can damage tissue. This risk is much higher with secondary Raynaud’s, which is why medical evaluation is important.
How Is Raynaud’s Diagnosed?
There is no single test that confirms Raynaud’s disease. Doctors typically rely on:
- A detailed description of symptoms
- How often episodes occur and what triggers them
- A physical examination
If secondary Raynaud’s is suspected, additional tests may be done to look for underlying conditions. The goal is not just to identify Raynaud’s, but to understand what may be causing it.
Managing Raynaud’s in Everyday Life
While there is no cure for Raynaud’s, many people successfully manage their symptoms with simple lifestyle changes.
- Keep warm: Gloves, warm socks, and layered clothing can help prevent attacks.
- Avoid sudden temperature changes: Gradual warming or cooling is gentler on blood vessels.
- Manage stress: Relaxation techniques, deep breathing, and mindfulness may reduce stress-related episodes.
- Protect your hands: Use insulated cups for cold drinks and wear gloves when handling cold items.
In more severe cases, doctors may prescribe medications that help relax blood vessels and improve circulation.
When Should You See a Doctor?
You should consider seeking medical advice if:
- Color changes happen frequently or are severe
- Only one hand or finger is consistently affected
- You experience pain, sores, or skin breakdown
- Symptoms begin suddenly later in life or worsen quickly
These signs may point to secondary Raynaud’s or another circulation issue that needs medical attention.
The Bottom Line
Seeing your fingers turn white or blue can be alarming, especially when it happens without warning. While cold weather is often the trigger, repeated episodes—particularly those linked to stress or mild temperature changes—may be a sign of Raynaud’s disease.
The good news is that, for many people, Raynaud’s is manageable. With awareness, lifestyle adjustments, and medical guidance when needed, most individuals continue to live full, active lives—without letting a little color change control their day.
Note: All images used in this article are AI-generated and intended for illustrative purposes only.
0 Comments