We’ve all been there: you wake up in the middle of the night, and your hand feels like a heavy, lifeless block of wood. Or perhaps you’re halfway through a long drive, and a strange, “fizzy” sensation begins to creep into your fingertips. At first, a tingling hand is easy to dismiss. We call it “pins and needles,” shake it out for a few seconds, and wait for the static to fade so we can get on with our day. Usually, this is just a temporary protest from a nerve that’s been squeezed or a brief drop in blood flow due to an awkward position.
However, tingling in the hand symptoms do not always stay harmless or occasional. When that numbness in your fingers refuses to leave, starts waking you from a deep sleep, or begins to climb up your arm, your body is no longer just complaining about a bad pillow—it is signaling a specific medical issue. Whether it arrives with weakness, burning pain, or a strange change in skin color, that “buzz” is a message. To decode it, we have to look at the patterns, the timing, and the specific fingers involved.
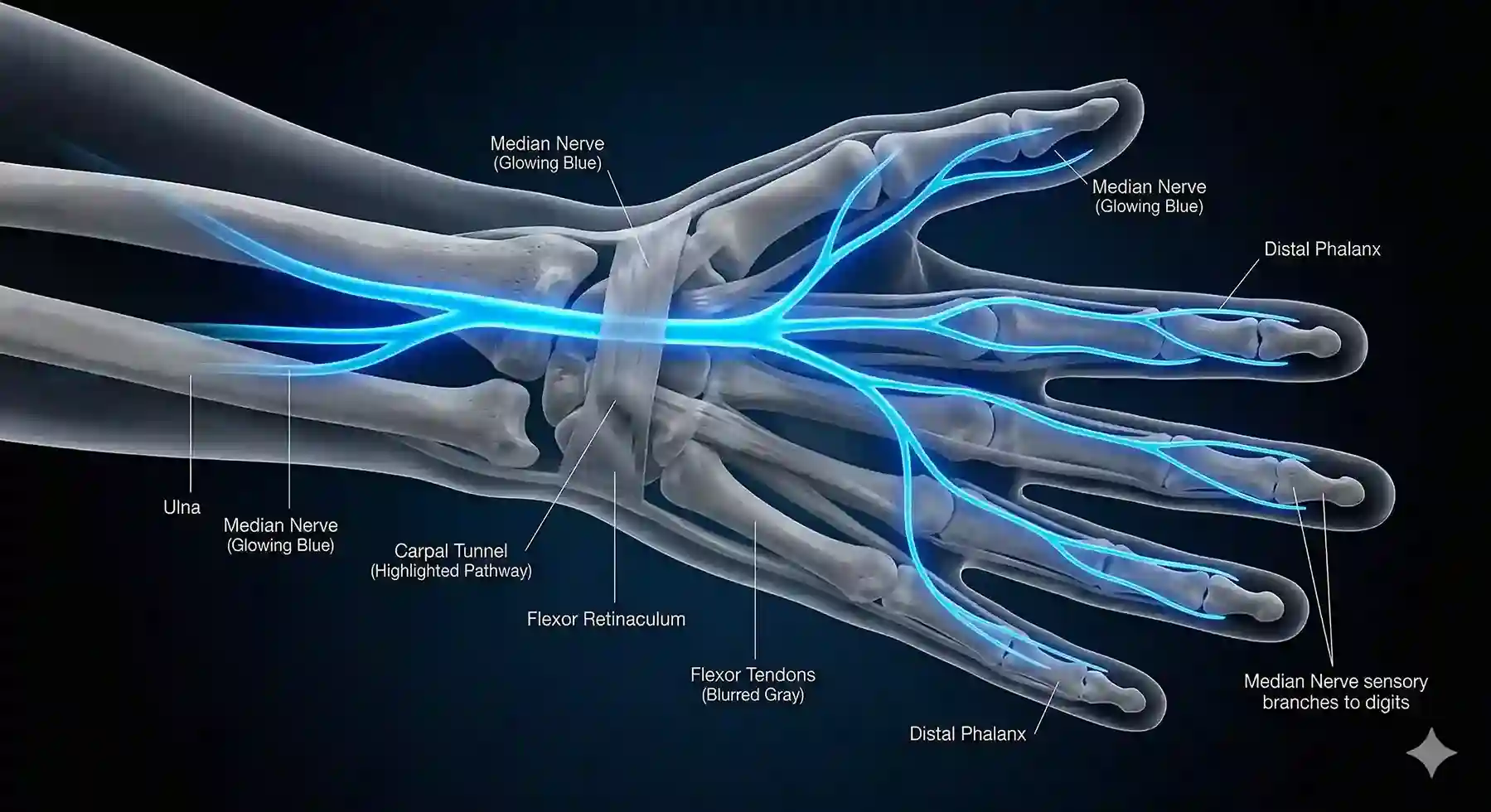
The median nerve acts as a high-speed data cable for your hand; when the tunnel narrows, the signal turns into ‘static.’
Carpal Tunnel Syndrome: The Most Common Culprit
When people think of hand numbness, Carpal Tunnel Syndrome (CTS) is usually the first name that comes to mind. According to the American Academy of Orthopaedic Surgeons (AAOS), it is an incredibly common condition that causes a suite of symptoms including numbness, tingling, pain, and even profound weakness in the hand and forearm. The anatomy of the problem is simple but frustrating: the median nerve, which provides sensation to most of your hand, must pass through a narrow, rigid “tunnel” in the wrist made of bone and ligament.
When the tissue inside this tunnel swells, the median nerve is caught in a vice. The distribution of the “fizz” is the biggest clue here. Typically, CTS affects the thumb, index finger, middle finger, and exactly half of the ring finger. If your pinky finger feels perfectly normal while the others are buzzing, you are looking at a classic case of carpal tunnel. These symptoms often build so slowly that many people ignore them until they start waking up at night feeling like their hand is “electrically charged” or burning. Tasks that require a sustained grip—like holding a phone, gripping a steering wheel, or reading a book—become triggers for the numbness.

Night-time symptoms are a hallmark of Carpal Tunnel Syndrome, often requiring the sufferer to ‘shake out’ the numbness to find relief.
As the condition progresses, the hand can become surprisingly clumsy. You might find yourself fumbling with buttons, dropping coins, or struggling to turn a key in a lock. Doctors urge early assessment because nerves are delicate; while they can recover beautifully if the pressure is eased early on, prolonged compression can lead to permanent muscle wasting and loss of sensation. Risk factors include diabetes, thyroid imbalances, pregnancy, and even the natural shape of your wrist. While repetitive work can aggravate it, CTS often develops without a single clear cause, making it important to monitor the “timing” of your symptoms regardless of your job.
Beyond the Wrist: The Elbow and the Neck
Carpal tunnel explains many cases, but it doesn’t explain them all. If your numbness is concentrated in your pinky and the outer half of your ring finger, the problem isn’t at your wrist—it’s likely at your elbow. This is known as Ulnar Nerve Compression or Cubital Tunnel Syndrome. The ulnar nerve (often called the “funny bone”) is easily irritated if you sleep with your elbows tightly bent or lean on armrests for long periods. Just like the median nerve, the ulnar nerve can lose its “signal” if squeezed for too long, leading to a loss of precision and grip strength.
Then there is the Cervical Radiculopathy—a fancy term for a pinched nerve in the neck. Your hand is essentially the end of a very long “electrical wire” that starts in your spine. If a disc in your neck is bulging or if arthritis has narrowed the exits for your nerves, the symptoms can travel all the way down to your fingertips. In these cases, you might notice that moving your neck in certain directions makes the hand tingling worse, or that placing your hand on top of your head (the “shoulder abduction sign”) actually makes it feel better. Because the source is in the neck, a wrist brace won’t help here; the assessment must look at the whole arm.
When Circulation Mimics Nerve Pain: Raynaud’s Phenomenon
Not every tingling hand is a “nerve” problem. Sometimes, it’s a “plumbing” problem. Your nerves need a constant supply of oxygenated blood to function; without it, they stop sending signals. Raynaud’s Phenomenon is a classic example of this. As explained by the National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS), this condition causes the blood vessels in the fingers to narrow violently in response to cold or stress.
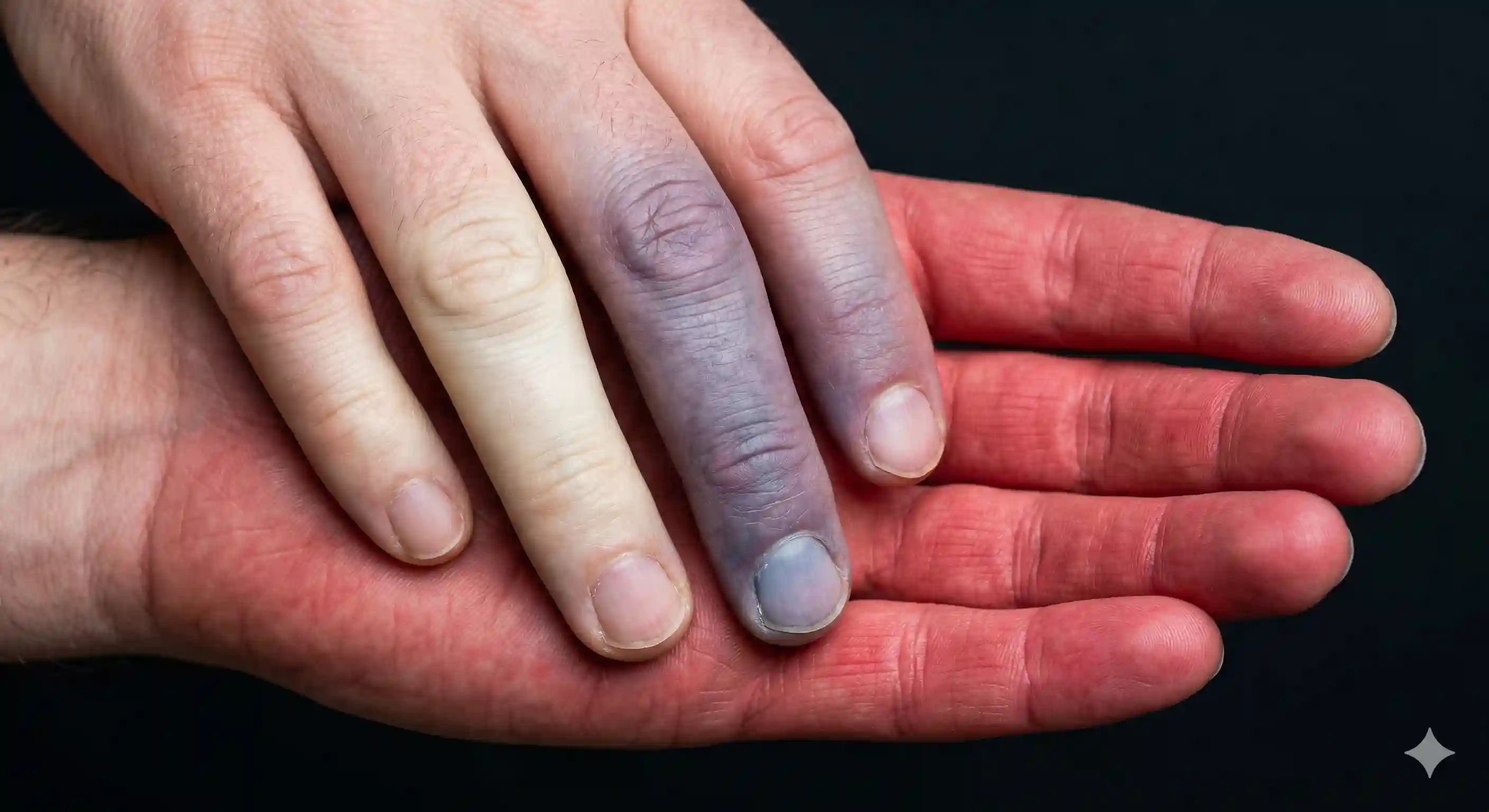
The dramatic color shift from white to blue to red is the hallmark of circulation-driven tingling.
During an attack, your fingers might turn a ghostly, waxy white as the blood leaves. They may then turn blue as the remaining oxygen is used up, and finally flush bright red as the blood rushes back in. This process is often accompanied by a sharp, throbbing, or burning “tingle” that is quite different from the “buzz” of carpal tunnel. While many people have “Primary Raynaud’s” (which is mild), others may have it as a symptom of an underlying autoimmune disease, making it important to track whether these attacks happen in both hands and if they lead to skin sores or ulcers.
Widespread Nerve Issues: Diabetes and Vitamin B12
When tingling starts in one hand and then spreads to both—or if it affects your feet at the same time—doctors look for systemic or metabolic causes. Diabetes is one of the most common drivers of peripheral neuropathy. Over time, high blood sugar levels can damage the delicate nerve fibers throughout the body. While it usually starts in the feet, the hands are often next. This type of numbness doesn’t follow a single nerve “map”; instead, it feels like a diffuse glove of numbness or burning pain that persists throughout the day.
Similarly, a Vitamin B12 Deficiency can wreak havoc on your nervous system. B12 is essential for creating the myelin sheath—the “insulation” that protects your nerves. Without it, your nerves start to “short circuit,” leading to tingling, balance problems, and even memory issues. This deficiency can be “silent” for years because the body stores B12, but once it appears, it can cause lasting damage if not treated. People on plant-based diets, those taking acid-reflux medication, or older adults with absorption issues are at the highest risk. A simple blood test can often solve a mystery that has lasted for months.
The Shoulder “Bottleneck”: Thoracic Outlet Syndrome
Sometimes the “traffic jam” for your nerves happens right at the base of your neck. Thoracic Outlet Syndrome (TOS) occurs when the space between your collarbone and your first rib is too tight, squeezing the nerves and blood vessels that serve your arm. This is a common cause for people who perform repetitive overhead tasks, like painters or shelf-stockers, or those who carry heavy backpacks. The “tingle” often starts at the shoulder and radiates down the inside of the arm to the hand. Posture plays a huge role here—slumping your shoulders can literally pinch the “hose” that supplies your hand with sensation.
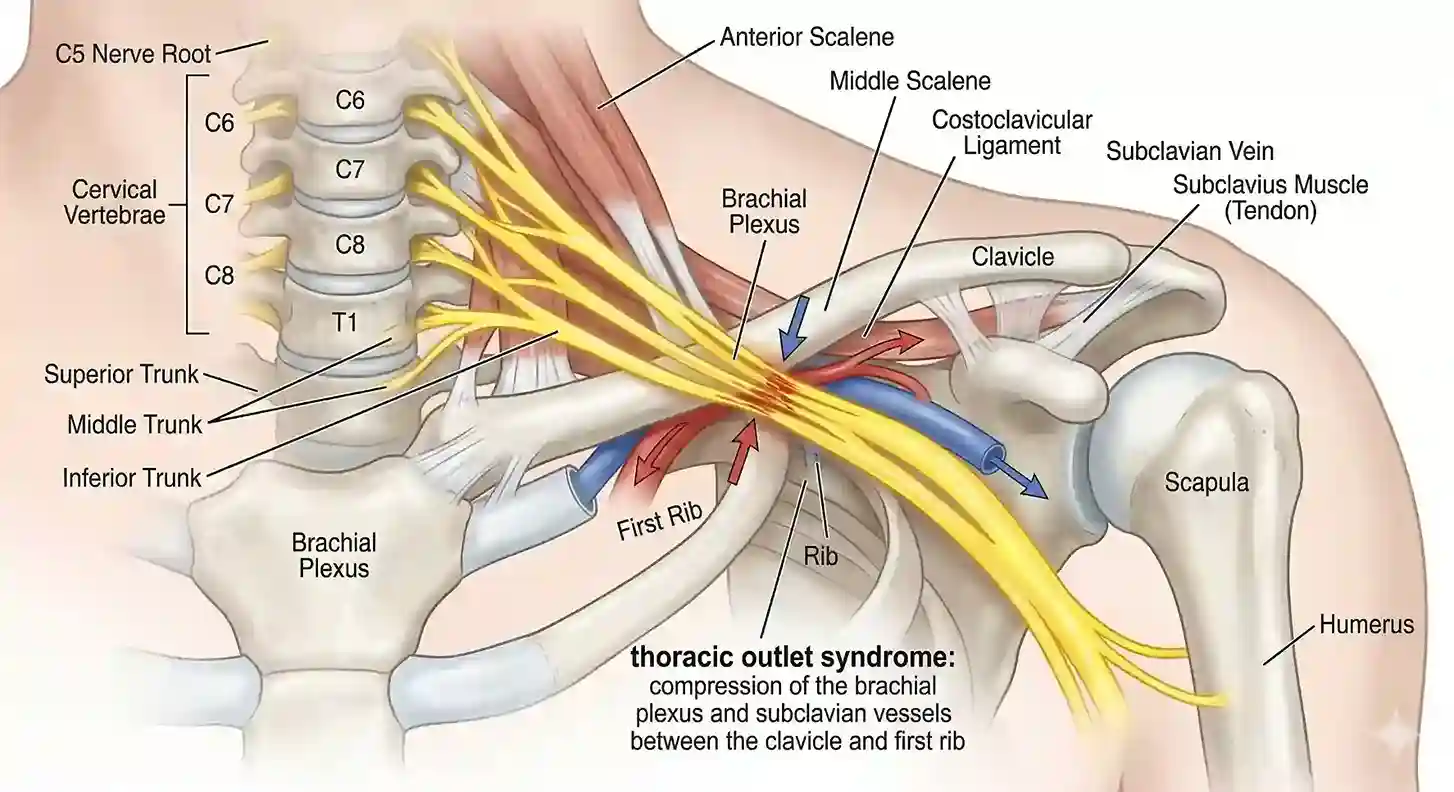
The thoracic outlet is a busy intersection for nerves; poor posture can lead to a literal nerve ‘gridlock.’
Structural Obstacles: Cysts and Injuries
In some cases, the hand tingles because there is a physical object pressing on a nerve. Ganglion cysts are the most common “lumps” found in the hand and wrist. While usually harmless, if they grow near a nerve pathway, they act like a physical barrier. These cysts can fluctuate in size—growing with activity and shrinking with rest—which explains why your hand might tingle one week and feel fine the next. Additionally, old wrist fractures or traumas can leave behind scar tissue or bone fragments that narrow the nerve’s path years after the original injury has healed.
The Role of the Thyroid
It surprises many to learn that an Underactive Thyroid (Hypothyroidism) can be a hidden cause of hand numbness. Thyroid hormones regulate the body’s chemistry and fluid balance. When these levels are low, the body can retain fluid, which increases the pressure within the confined spaces of the carpal and cubital tunnels. If your hand tingling is joined by symptoms like unexplained weight gain, constant fatigue, cold intolerance, or dry skin, the “fix” might lie in balancing your hormones rather than wearing a wrist splint.
When to Seek Urgent Medical Care
While most hand tingling is a chronic, slow-moving issue, some patterns require a trip to the Emergency Room. Sudden numbness, especially if it only affects one side of the body, can be a sign of a stroke or a Transient Ischemic Attack (TIA). If the tingling arrives alongside facial drooping, difficulty speaking, sudden confusion, or trouble walking, do not “wait and see.” Time is critical in preventing lasting brain damage.

Recognizing ‘Sudden Onset’ symptoms can be a life-saving skill. Never ignore one-sided numbness.
Even in non-emergency cases, you should seek a professional opinion if your hand tingling is constant, if you are losing muscle mass in the “meaty” part of your palm, or if the numbness is making it dangerous for you to hold objects or drive. By keeping a “symptom diary”—noting which fingers tingle, what time of day it happens, and what activities trigger the sensation—you can help your doctor narrow down the cause much faster. Remember: tingling is a symptom, not a diagnosis. Tracing it back to its source is the first step toward reclaiming the full use of your hands.
Disclaimer: Content is provided for informational purposes only and is not intended as a substitute of medical advice. Seek guidance of your doctor regarding your health and medical conditions.
Note: All images used in this article are AI-generated and intended for illustrative purposes only.
0 Comments